The Lawrence Clinic, Pudsey has a long and established Chiropody treatment department provided by Jonathan Stanley D.Pod.M.,MChS Podiatric Medicine who is registered with The Health Professions Council and The Society of Chiropodists & Podiatrists.
Also Dan Broadley and Emer McConomy who are also state registered podiatrists who works as part of the team.
Chiropody treatment will cover everything from Diabetic clinics to toenail cutting or hard skin removal or corn removal. We also assess the foot health as part of our treatment regime. We do offer Home visits for housebound patients.


Chiropody Treatment for Corns and Callus
Callus
When we walk or stand, our body weight is carried first on the heel and then on the ball of the foot, where the skin is thicker, to withstand the pressure. When this pressure becomes excessive, some areas of the skin thicken, in the form of corns and callus, as a protective response.
A callus, or callosity, is an extended area of thickened skin on the soles of the feet, and occurs on areas of pressure. It is the body’s reaction to pressure or friction, and can appear anywhere the skin rubs against a bone, a shoe, or the ground.
Walking on stones?
Most calluses are symptoms of an underlying problem like a bony deformity, a particular style of walking, or inappropriate footwear. Some people have a natural tendency to form callus because of their skin type. Elderly people have less fatty tissue in their skin and this can lead to callus forming on the ball of the foot.
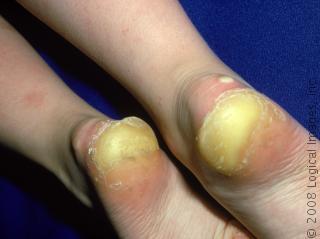

Chiropody Treatment – what to do
You can control a small amount of hard skin by gently rubbing with a pumice stone, or chiropody sponge occasionally when you are in the bath. Use a moisturizing cream daily. If this does not appear to be working, seek advice from a registered chiropodist (also known as podiatrist) or pharmacist
If the callus is painful and feels as if you are “walking on stones”, consult a registered chiropodist/podiatrist who will be able to advise you why this has occurred and, where possible, how to prevent it happening again. Your chiropodist/podiatrist can also remove hard skin, relieve pain, and redistribute pressure with soft padding, strapping, or corrective appliances which fit easily into your shoes. The skin should then return to its normal state.
The elderly can benefit from padding to the ball of the foot, to compensate for any loss of natural padding. Emollient creams delay callus building up, and help improve the skin’s natural elasticity. Your chiropodist/podiatrist will be able to advise you on the most appropriate skin preparations for your needs.
Corns
When we walk or stand, our body weight is carried first on the heel and then on the ball of the foot, where the skin is thicker, to withstand the pressure. When this pressure becomes intense, growths, in the form of corns and callus, may appear.
Corns more often occur over a bony prominence, such as a joint.
There are five different types of corns. The two most common are hard and soft corns.


HARD CORNS
These are the most common and appears as small, concentrated areas of hard skin up to the size of a small pea, usually within a wider area of thickened skin or callous, and can be symptoms of feet or toes not functioning properly.
SOFT CORNS
These develop in a similar way to hard corns. They are whitish and rubbery in texture, and appear between toes, where the skin is moist from sweat, or from inadequate drying. A registered podiatrist/chiropodist will be able to reduce the bulk of the corn, and apply astringents to cut down on sweat retention between the toes.
SEED CORNS
These are tiny corns that tend to occur either singly or in clusters on the bottom of the foot. They are usually painless.
VASCULAR CORNS
These corns will bleed profusely if they are cut and can be very painful.
FIBROUS CORNS
These arise from corns that have been present for a long time. They appear to be more firmly attached to the deeper tissues than any other corn. They may also be painful.
WHAT TO DO
Don’t cut corns yourself, especially if you are elderly or diabetic, and don’t use corn plasters or paints which can burn the healthy tissue around the corns. Home remedies, like lambswool around toes, are potentially dangerous. Commercially available ‘cures’ should be used only following professional advice.
You could use a pumice stone to remove the thickened skin a little at a time, or relieve pressure between the toes with a foam wedge, but if you are unsure of what to do, or need special attention, consult a registered podiatrist/chiropodist for advice on treatment , we have 3 Podiatrists at our clinic and we can help with all aspects of treatment for the foot and lower limb pain.
Verruca management
What is a verruca? A verruca is simply a wart that is usually found on the soles of your feet, though they can also appear around the toes. In the early stages, a verruca looks like a small, dark, puncture mark but later turns grey or brown. It may become rough and bumpy with a cauliflower-like appearance and may develop a black spot in the middle, which is caused by bleeding. A verruca can grow to half an inch in diameter and may spread into a cluster of small warts.
What causes them? Verrucae are caused by the human papiloma virus (HPV). This virus is very contagious, but can only be caught by direct contact. It thrives in warm, moist environments such as swimming pools, changing room floors and bathrooms. So if an infected bare foot walks across the poolside, it may release virus-infected cells onto the floor. If you then walk on the same floor, you can pick the virus up, especially if you have any small or invisible cuts and abrasions that make it even easier for the virus to penetrate. You could also catch the virus from an infected towel.
Is it serious? Verrucae are harmless however, they can cause a sharp, burning pain if you get one on a weight-bearing area such as the ball or the heel of the foot. Because you are constantly pressing on the area when walking, they can protrude into the skin and become more painful.
When you have verrucae on a non-weight-bearing surface (such as on the top of the foot or on the toes), they protrude above skin level, tend to be fleshier and cause less pain.
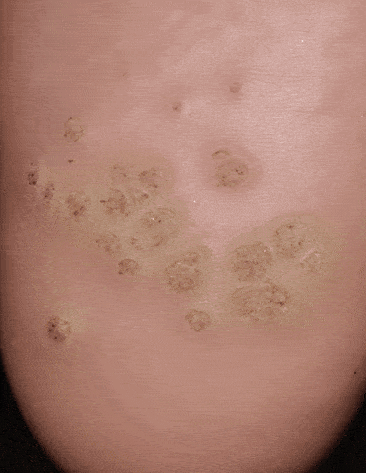

Who gets them? Then tend to be common in children, especially teenagers. However, for unknown reasons, some people seem to be more susceptible to the virus, whereas others are immune.
What’s the difference between a corn and a verruca? A verruca is a viral infection, whereas a corn or callus are simply layers of dead skin. Verrucae tend to be painful to pinch, but if you’re unsure, your podiatrist will know.
What can I do? Minimise your chances of catching a verruca by keeping your feet clean and dry, and covering up any cuts or scratches. Avoid walking barefoot in communal showers or changing rooms (wear flip-flops) and don’t share towels. Though you should wear verruca socks when swimming to avoid passing on the virus, they can also be worn as a preventive measure.
If a verruca does appear, avoid touching or scratching it as it may spread into a cluster of several warts. Instead, cover it up with plaster. In some cases, this may cure it.
Do not self-treat if you have diabetes or circulation problems. However, if you are fit and healthy, it’s fine to treat yourself with over-the-counter gels and ointments. Ask your pharmacist for advice or look for products containing salicylic acid, such as Verigin. Ensure, however, that you follow the instructions carefully. If, at any stage, your verruca becomes painful or the surrounding skin goes red, stop treatment immediately and see a podiatrist. If you damage the healthy tissue that surrounds the wart tissue you could hamper further treatment.
What can a podiatrist do? Because verrucae usually often disappear in time (fought off by your immune system), the general policy in the UK is to only treat them when they are causing pain. Verrucae generally resolve spontaneously within six months in children. But in adults, they can persist for years.
If yours is causing pain, there are a number of treatment options available – though no one particular treatment can guarantee a cure. A recent review of treatments in the British Medical Journal (August 2002) concluded that the safest and most effective treatments were those containing salicylic acid. This acid is applied to the wart to disintegrate the viral cells and has a cure rate of 75%. It may need to be applied at weekly intervals over a set period of time.
Other treatments include:
Cryotherapy This involves freezing warts off with liquid nitrogen or nitrous oxide gas. This needs to be done every 2 or 3 weeks for a few months before the verruca is fully removed. However, it can lead to soreness and blistering in some people. You can still swim after this treatment, but it’s not advised for sensitive or anxious children.
Excisional Surgery Under local anaesthetic, the verruca is pared down and a full thickness of skin is excised with the verruca intact, it should be noted that around 20% of those warts removed this way may return.
In short, you can treat your verruca with an over-the-counter medicine unless you have diabetes or circulation problems. If you do however, or find that the verruca appears to be getting bigger, consult a podiatrist.
Diabetic foot assessments clinic
One of the first ways in which diabetes may affect your feet is through the loss of sensation within your feet, often starting at the toes. You may experience a cotton wool like feeling or numbness in your feet, this is called neuropathy.
Your chances of losing feeling in your feet increases with the number of years that you have diabetes and research suggests that up to one in three people with diabetes have some loss of sensation (called neuropathy). The onset of neuropathy is gradual and often people who develop this complication are unaware of it in the beginning. Often it occurs between 7 and 10 years of having diabetes, although in some cases it can occur sooner where blood sugar levels have not been so well controlled.
If you have lost feelings in your feet then it is possible that you may unknowingly damage your feet. You may stand on sharp objects like a nail, piercing the skin even down to the bone without realising. If unnoticed and not treated appropriately this can have potentially serious consequences and could lead to an amputation. Such an outcome is less likely if you seek expert advice from your multi-disciplinary foot team.
This explains why your podiatrist checks your ability to feel pressures on the soles of your feet and toes every year. If you are forewarned that you have lost or are losing feeling then you will be able to reduce the risk of problems occurring by undertaking daily inspections of your feet and taking precautions such as not walking bare footed or sitting too close to fires.
Occasionally people with loss of feelings can sense a burning pain in their feet. This can be severe and worse at night, they can find contact from socks and shoes can cause discomfort. This is called painful peripheral neuropathy. If you experience these symptoms it is advisable to consult your Diabetic Clinic or Podiatrist, it is possible in many cases to alleviate the symptoms.
Diabetes can also affect blood supply to and within your feet, this can delay healing and increase your risks of infection. Because the implications of poor blood supply can have serious consequences for your feet, your podiatrist will need to routinely screen your feet for signs of poor blood flow. If necessary you may be referred on to a Vascular Surgeon. Our facilities allows us to check your blood flow and do a range of tests as part of your Diabetic foot health.
Chiropody home visits:
Home visits for chiropody services are now available with our chiropodist Emer McConomy!
Please note: We are only taking home visit appointments from patients who live within a 3 mile radius of the clinic.



